Examination Date: 2014-03-14
Intermediate Exam
Chief Complaint
1. Left Lower Back
Here is an example of a patient with subacute lower back pain. Occasional left lower back pain. Patient reports over all improvement, less pain and has returned to modified hours at work. She considers this complaint as moderate and rated the pain as a 5 on a scale of 0 to 10 with 10 being the worst. The pain is described as sharp, occurs most often after moderate physical activities and in the morning and is radiating into the left buttock, left calf and left hip. The pain is reduced by range of motion and chiropractic treatments while bending and prolonged standing aggravates the condition. Further concerns of this condition are tingling.
Capabilities of Daily Living
The patient states that capabilities of daily living have been affected in the following areas:
I am unable to lift heavy objects off the floor. However, I can manage if they are at table height. I am restricted to social activities at home due to pain. I experience MODERATE pain, which causes a significant limitation on my physical performance of activities. Pain is FREQUENT, and occurs between 50% and 75% of my awake time.
Physical Examination
Physical examination revealed an individual who was alert, cooperative and orientated.
The patient had a limping gait. The limp appeared on the right. Minor’s sign was positive.
Sex: Female
Age: 33
Height: 165 cm
Weight: 70 kg
BMI: 25.7
Complexion: Normal
Size: Normal
Grip strength: Normal bilaterally.
Posture
There is no indication of a head tilt in the patient’s posture. Ms. XXXX shoulder level appeared high on the left. There is no evidence of a forward head carriage. Observation and inspection of the thoracic spine revealed a normal spine. Profile view of the lumbar spine revealed normal curvature. Romberg’s test was negative. Adam’s sign was negative. Left heel walk: WNL. Left toe walk: WNL.
Ranges of Motion
Lumbar Spine
Motion Degree Normal Pain Level
Flexion: 42 60 Mild
Extension: 16 25 Moderate
Lateral Right: 25 25 No
Lateral Left: 21 25 No
Neurological Testing
Reflexes Wexler’s Grading System
L R
Patellar (L2, 3, 4) 1+ 2+
Achilles (S1, 2) 2 2
Jendrassik was not required.
Lower Extremities:
Left Right
L-4 Decrease
L-5 Decrease
S-1 Equal
Lumbar Spine Evaluation
Lumbar spine evaluation provided the following results:
Palpation of the spine indicated discomfort and pain in the spinous process at: L4 and L5 (grade 3). Straight leg raise was positive on the left (60 deg). The patient also reported experiencing radiating pain during the test. Straight leg raise was negative on the right (90 deg). Kemps was positive on the left. Kemps was positive on the right. Shear stability test was positive at L4 level.
Lower Extremities Muscle Testing
Tibialis 5/5 5/5
Extensor Hallucis Longus 4/5 5/5
Hamstrings 5/5 5/5
Peroneous Longus 5/5 5/5
Ms. XXXX demonstrated L5 (big toe extension) of 7 lbs on the right and 4 lbs on the left.
Diagnosis
M5416 Radiculopathy, lumbar region
Acute, moderate to severe traumatic joint and muscle dysfunction in the above region with associated symptoms of pain, ROM reduction and functional difficulties. Radiculopathy consitent with MRI findings of small central disc herniation at L4-L5, mild DJD of L4-L5 and L5-S1 and disc bulge at L5-S1.
Management Plan
Short Term Goals would be for Ms. XXXX to report 50% pain reduction and 50% increase in ROM within 2 weeks. Functionally Ms. XXXX should also be able to perform half of her ADL’s within these 2 weeks easier. Long Term Goals would be for Ms. XXXX to report over 80% pain reduction and demonstrate over 80% increase in ROM within 4 to 6 weeks. Functionally Ms. XXXXX should also be able to perform most of her ADL’s within this period. Ms. XXXX is also to be discharged with a home exercise program when the above goals have been achieved and she is over 80-90% impairment free.
Spinal Decompression 3x per week/duration of 3 weeks (to stabilize lumbar spine in a pain free manner)
Lumbar stability exercises 3x per week/duration of 3 weeks (to stabilize lumbar spine in a pain free manner)
Today’s Treatments
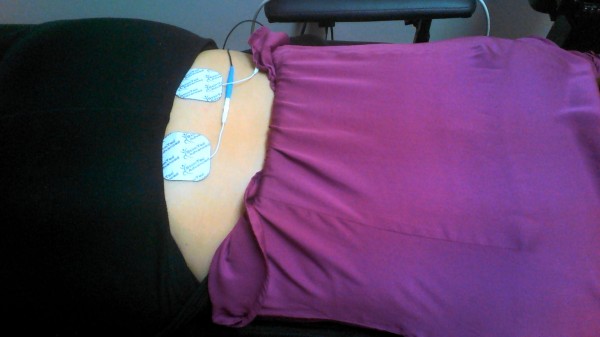
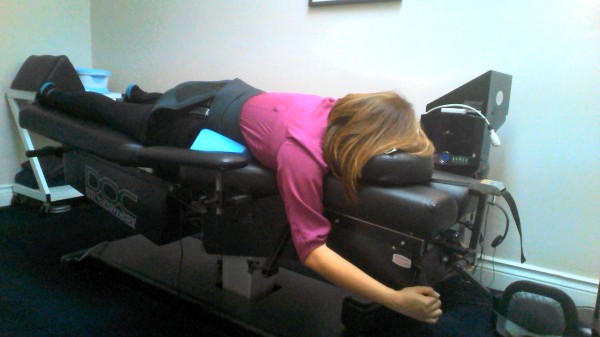
Today’s treatment consisted of Electrical Stimulation in the lumbar region; Chiropractic Spinal Decompression (Pron,6,60 lbs,-7deg and20min NP) in the lumbar region. Proper use of heat or ice, sitting, standing, transferring, lifting, pushing and sleeping was explained to Ms. XXXXX today.
Prognosis
The prognosis for improvement of the patient’s condition is considered good.
Notes:
She has L4 spinous process pain during 2 lbs shear provocation test. She has positive findings of disc herniation and DJD in lower lumbars. Although she had more pain during extension, I still think extension is a better position for her.
DOC Settings:
Prone: It is the go-to position, plus as you can see IFC can be added at the same time to reduce muscle spasm.
Protocol: 6 with frequent pulls at the early treatments
Force: She is 70 Kg or 154 Lbs so 60 lbs is a good starting point.
Angle: I choose -7 to give her some centralizing extension. Patient was asked if they have any pain or radiation or discomfort and she was ok.
Proper use of heat or ice, sitting, standing, transferring, lifting, pushing and sleeping was explained to the patient.
Also Read
| Case Study: Acute Lumbar Radiculopathy (2) | Case Study: Subacute Lower Back Pain | Case Study: Chronic Lower Back Pain | Case Study: L5-S1 Disc Prolapse |
| Case Study: Lumbar Spinal Stenosis | Case Study: Right lateral disc protrusion at L5-S1 | Case Study: Antalgic Posture | Peroneal (Lower Leg) Tendonitis |
| Low Back Osteoarthritis | Low Back Pain |