Lumbar Spinal Stenosis (2)
Initial Exam
Chief Complaints
- Bilateral Lower Back
Frequent bilateral lower back pain. Patient reports insidious onset of the complaint for the past 1.5 years. He regards this complaint as moderate and rated the pain as a 6 on a scale of 0 to 10 with 10 being the worst. The pain is explained as aching and dull and radiates into the left buttock, left hip, right buttock and right hip. The pain is relieved by resting while bending, lifting, prolonged standing and prolonged walking worsens the condition.
History
Mr. XXXXXX states that he currently has diabetes. Patient has prostate surgery in 1995. Patient’s reported that his father had a stroke.
Capabilities of Daily Living
The patient states that capabilities of daily living have been affected in the following areas:
Due to pain, I am not able to lift heavy objects. However, light to medium weight objects are manageable. I experience MODERATE pain, which causes a significant limitation on my physical performance of activities. Pain is FREQUENT, and occurs between 50% and 75% of my awake time.
Physical Examination
Physical examination revealed an individual who was alert, cooperative and orientated.
The patient’s gait appeared normal. Minor’s sign was negative.
Sex: Male
Age: 68
Height: 180 cm
Weight: 104 kg
BMI: 32.1
BP: 112/60
Pulse: 82/bpm
Complexion: Normal
Size: Overweight
Grip strength: Normal bilaterally.
Posture
There is no indication of a head tilt in the patient’s posture. There is no evidence of a forward head carriage. Observation and inspection of the thoracic spine revealed a normal spine. Profile view of the lumbar spine revealed normal curvature. Romberg’s test was negative. Adam’s sign was negative. Left heel walk: WNL. Right heel walk: WNL. Left toe walk: WNL. Right toe walk: WNL. Trendelenberg test on the left was negative. Trendelenberg test on the right was negative.
Ranges of Motion
Lumbar Spine
Motion Degree Pain Level
Flexion: Moderately Decreased Moderate
Extension: Moderately Decreased Moderate
Lateral Right: Moderately Decreased Moderate
Lateral Left: Moderately Decreased Moderate
Neurological Testing
Reflexes Wexler’s Grading System
L R
Patellar (L2, 3, 4) 1+ 1+
Achilles (S1, 2) 1+ 1+
Lower Extremities:
Left Right
L-4 Equal
L-5 Equal
S-1 Equal
Lumbar Spine Evaluation
Lumbar spine evaluation provided the following results:
Evaluation of the lumbar spinal region reveals tender areas in the lumbar region on both sides (grade 2) and erector spinae on both sides (grade 2). Palpation of the spine indicated discomfort and pain in the spinous process at: L4, L5 and S1 (grade 2). Evaluation of the lumbar spinal areas indicates that trigger points are present in the erector spinae bilaterally (moderate) and quadratus lumborum bilaterally (moderate). Kemps was positive on the left. The patient reported localized low back pain during the test. Kemps was positive on the right. The patient reported localized low back pain during the test. The following lumbar orthopedic tests were positive: SLR passive on both sides. Kemps test was positive for possible facet and meniscoid entrapment.
X-Ray Analysis
Lumbar
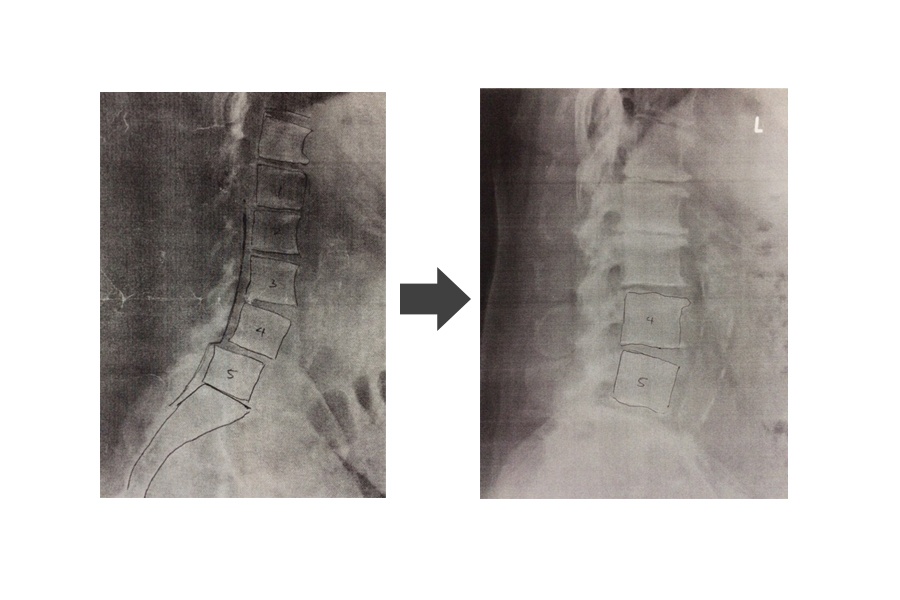
The following views were taken: A-P and lateral. Radiographic results showed evidence of osteoarthritis. The lumbar curvature demonstrates a mild loss of the normal lordosis. There is a grade 1 anterolisthesis at L4-L5. There is anterior lipping and spurring at L3-L4. There is moderate loss of the intervertebral disc height at L1-L2. There is severe loss of the intervertebral disc height at L5-S1.
Impression
Severe DJD at L5-S1, moderate L1-L2. Anterolesthesis about 25% of L4 on L5.
Diagnosis
M545 Low back pain
M5416 Radiculopathy, lumbar region
Spinal stenosis. Acute, moderate to severe traumatic joint and muscle dysfunction in the above region with associated symptoms of pain, ROM reduction and functional difficulties.
Diagnostic/X-Ray Requests
The following diagnostic procedures have been ordered by the clinician after medical/clinical necessity has been established:
Radiographs are being ordered to identify any gross pathologies, fractures or joint degeneration, as well as over all alignment of the segment.
Today’s Treatments
Today’s treatment consisted of laser therapy (Class IV 350J) in the lumbar region; Spinal Decompression (Supine,6,80 lbs,-10deg and 20min NP
) in the lumbar region. YYYYY endured these treatments with mild pain. Proper use of heat or ice, sitting, standing, transferring, lifting, pushing and sleeping was explained to Mr. XXXXXX today.
Prognosis
The prognosis for improvement of the patient’s condition is considered fair.
Notes:
This patient attended our clinic for a full year. There were over 30 visits. No exercises was given. He was treated solely with spinal decompression and Laser and other modalities. Since he was diagnosed with spinal stenosis supine with 10 degrees of flexion was chosen. 80 lbs and 20 minutes also was performed given patient’s weight and severity of original pain. Patient felt better after the third visit. After the 10th visit the frequency of treatments was reduced to once a week from three time a week. After 20 visits the frequency of treatments was reduced again to once every 2 weeks. Patient reported to be virtually pain free after 20 visits. However to avoid return of symptoms he decided to continue treatments once every two weeks. A new set of radiographs reveal significant improvement in anterolisthesis of L4 on L5, exactly one year later.